
You walk onto a new unit on day one of a locums gig. Everyone seems to know where to go, who to page, the exact unspoken rules about when rounds really start and which nurse hates being called after 10 p.m. You don’t even know where the bathrooms are.
You’re wearing the badge, you’re technically “the doctor,” but inside you feel like the substitute teacher no one takes seriously. The outsider doctor. The temp. The easy scapegoat if something goes wrong.
And you’re thinking: what if they don’t trust me? What if I miss some unwritten rule and look incompetent? What if the nurses test me? What if this follows me and ruins my reputation?
You’re not crazy for thinking that. Locum tenens after residency can feel like walking into someone else’s family dinner every few weeks and being told, “Act natural.”
Let’s talk about how this actually plays out, what’s real vs what’s just anxiety spiraling, and how to walk in as a locum without feeling like you’re permanently on probation.
The “Outsider Doctor” Fear: You’re Not Imagining It
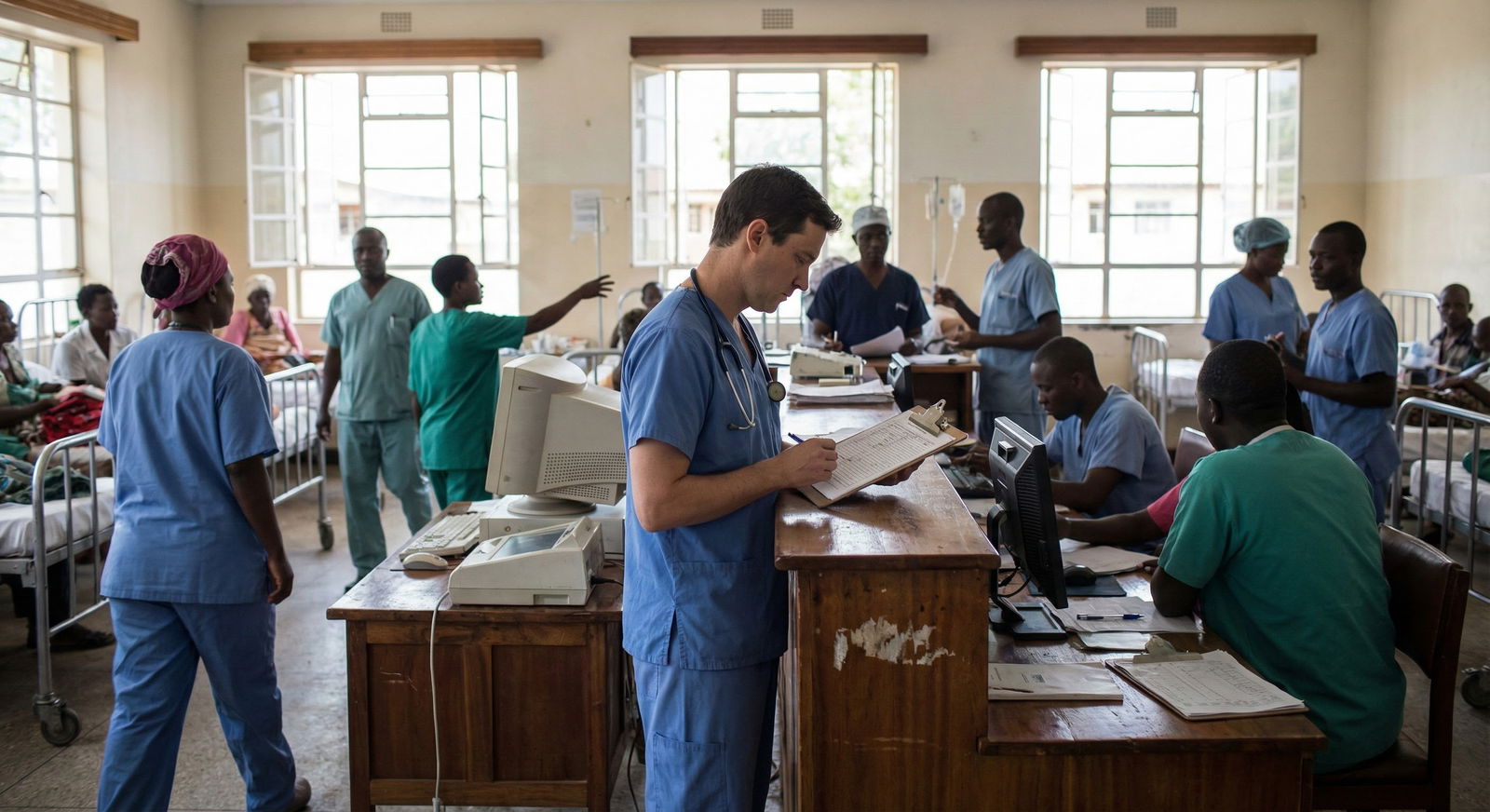
There’s this thing no one really warned you about in residency: how much of medicine is vibes and culture, not just knowledge.
In your home program, you knew:
- Which attending wanted 10-line notes vs 3 sentences
- Which nurse practitioner would quietly fix your orders vs page you at 3 a.m.
- How to get something done when “the system” said no
In locums, you walk in with:
- No history
- No shared war stories
- No institutional memory
So yeah, you feel exposed. It’s not just “new job nerves.” It’s that you’re literally missing a whole chunk of unwritten information everyone else has.
Here’s the part that messes with your head: staff often do initially treat you like an outsider. Because to them, you are. They’ve seen temps come through who:
- Didn’t know the EMR and slowed everyone down
- Were clinically fine but arrogant
- Were clearly there just for the paycheck
So you’re walking into mild skepticism + your own anxiety. That’s the combo.
But I’m going to say this bluntly: being “the outsider doctor” is a phase, not an identity. You just need to survive the first 3–5 days without letting your brain convince you you’re a fraud.
What Teams Actually Care About (It’s Not What You Think)

| Category | Value |
|---|---|
| Responsiveness | 90 |
| Safety/Asking for Help | 85 |
| Respect for Staff | 80 |
| Speed | 60 |
| Personality | 50 |
You’re probably worried about all the wrong things.
You’re obsessing over:
- “Do I look dumb if I ask where something is?”
- “Do they think my training was good enough?”
- “Am I as fast as the regular attendings?”
But most teams are actually clocking you on a different scale:
Are you safe?
Not perfect. Not genius. Safe. Do you ask for help when you should? Do you double-check high-risk stuff? Do you say “I’m not familiar with your protocol—can you walk me through it?” instead of winging it?Are you respectful?
Do you talk down to nurses or act like the EMR is beneath you? Or do you say, “I know I’m the new one here, please stop me if I’m doing something that doesn’t fit your process”?Are you reachable?
They hate locums who disappear. If you answer your pages, round when you say you will, and own your decisions, you move from “outsider” to “reliable” very fast.Do you make their life harder or easier?
You don’t have to be beloved. Just not a walking headache.
I’ve watched units warm up to locums who were very average clinically but rock solid on communication and humility. I’ve also seen brilliant people frozen out because they came in defensive and rigid.
Walking In On Day One Without Imploding

| Step | Description |
|---|---|
| Step 1 | Arrive Day One |
| Step 2 | Meet Charge Nurse |
| Step 3 | Ask Preferred Communication |
| Step 4 | Identify Key Allies |
| Step 5 | Clarify Protocols |
| Step 6 | Round Consistently |
| Step 7 | Ask for Feedback Day 3 |
Day one feels like your whole career is being judged. It’s not. But the first impression does matter. Here’s how to stack the deck in your favor without fake-smiling your way into burnout.
Script your opening
Do not wing this. When you first meet the charge nurse and unit staff, say something like:
“Hi, I’m Dr. ___. I’m here with locums for the next ___ weeks. I’m still learning your system, so if I do something that doesn’t fit your usual flow, please tell me. I’d rather be corrected early than frustrate you guys.”
That line does three things:
- Lowers their defensiveness
- Signals you’re not arrogant
- Gives them permission to guide you (which many actually like)
Identify your “anchor people”
Within the first 24 hours, you want to know:
- Who’s the charge nurse everyone listens to?
- Who’s the go-to resident/PA/NP who actually knows how stuff works?
- Who’s that one unit secretary/ward clerk who can find anything and everyone?
These 2–3 people are your lifeline. You don’t need to win over all 40 staff. Just get a few humans who don’t hate you.
Something as simple as:
“Hey, you clearly know how things really work here—if I have a stupid question about workflow, can I ask you?”
You’d be amazed how far that goes.
Over-communicate early
First 3–5 days, you’re allowed to be “that doctor who explains too much” instead of “that doctor who disappears.”
Say things out loud like:
- “I’m going to check on room 12 again in an hour because I changed x.”
- “I’ll be on the unit until 6 p.m., then on pager the rest of the night.”
- “I’m not familiar with how you handle borderline ICU patients—do you usually talk to intensivist early, or only at certain thresholds?”
You’re showing them you’re predictable and safe. That buys you forgiveness for being slow or asking extra questions.
Common Locum Nightmares (And What Actually Happens)

Your brain is probably running worst-case scenarios. Let me walk through a few and be blunt about which are real, which are exaggerated, and what you can actually do.
“They’ll treat me like I’m incompetent because I’m locums.”
Reality: Some will be skeptical. A few will be jerks. Most are neutral and waiting to see which category you fall into.
Fast ways to get labeled competent (even if you feel shaky inside):
- Admit what you don’t know about their system
- Be decisive about medical decisions once you have the info
- Own mistakes quickly: “I ordered X when I should’ve done Y—thanks for catching that.”
Teams see so many doctors come and go that they’re actually pretty quick at recalibrating their opinion. If day one is rocky but day three you’re communicating well and not doing reckless stuff, you’ll feel the tension drop.
“The staff all know each other and I’ll always be the outsider.”
First week? You will feel like the extra. That fades.
Humans are lazy. Once you’ve been around a bit, people default to normal patterns: small talk, inside jokes, “good morning doc.” You don’t have to become work-best-friends. You just need to move from “unknown quantity” to “part of the background.”
If you’re somewhere for a few weeks or months, this usually happens:
Week 1: Who is this? Why are they so slow with the EMR?
Week 2: Okay, they’re fine. They answer pages.
Week 3+: “Oh, Dr. ___ is back on—cool, they’re reasonable.”
“If I mess up once, I’ll be blacklisted forever.”
Is there reputational risk? Yes. Medicine has a long memory for people who are unsafe, dishonest, or toxic.
But one awkward patient interaction, one slightly delayed order, one night where you were overwhelmed? That’s not getting you blacklisted. Staff are used to imperfection. What freaks them out is:
- Blaming others
- Refusing to acknowledge issues
- Being defensive when given feedback
If something goes sideways, your script is:
- Acknowledge: “You’re right, that could’ve gone smoother.”
- Clarify: “Here’s what I was thinking at the time.”
- Adjust: “Next time I’ll loop you in earlier / change X / do Y.”
Mature response = huge credibility boost.
Concrete Tactics To Stop Feeling Like a Permanent Temp
| Situation | What You Can Say/Do |
|---|---|
| First meeting charge nurse | Ask about rounding norms and call preferences |
| Unsure of local protocol | Explicitly ask for their standard process |
| EMR confusion | Admit it and ask superuser for a 10-min run |
| Getting pushback | Validate concern, restate plan clearly |
| End of first week | Ask 1–2 staff if anything is frustrating |
This is the part where I stop hand-waving and just give you tactics.
1. Learn their non-negotiables quickly
Every place has a few things they care about way more than others:
- The ICU attending who wants to be notified for every lactate > x
- The meds that MUST be ordered certain ways in the EMR
- The sacred rule about never writing “DC Foley” without x criteria
Ask directly:
“Every place has those 3–5 things that people get really upset about if you don’t do them the standard way. What are those here?”
You’ll look smart, not clueless.
2. Use the “new doc” card strategically
You are new. Use it—without weaponizing it as an excuse.
Good uses:
- “I’m still getting used to your admission order sets, so if something looks off, please tell me.”
- “I’m not sure who usually handles X—can you point me to the right person?”
Bad uses:
- “I didn’t know, I’m just the locums doc.”
- “This is how we did it at my hospital; I guess your way is different.”
You want humility, not helplessness.
3. Pre-empt the “locum = lazy” stereotype
A few easy habits help:
- Round when you say you will. Don’t be “flexible” with time the first week.
- If you step off the unit, tell someone: “I’ll be in my office for 30 minutes finishing notes, page me if anything urgent comes up.”
- Don’t vanish right at shift change if there’s a mess brewing. Help with the transition, then leave.
You don’t need to martyr yourself. Just don’t act like you’ve punched a time clock at 4:59 p.m. while someone is coding down the hall.
4. Ask for tiny, specific feedback
Do not say, “How am I doing?” They’ll just say, “Fine.”
Instead:
“I know I’m still getting used to this place—has anything about my workflow been frustrating you or the team?”
Or even narrower:
“Is there anything I could do that would make your day on this unit smoother? Even something small.”
You might hear:
- “If you could sign your notes before noon, that’d help a lot.”
- “We prefer if you update families earlier in the day.”
Small adjustments. Huge relational payoff.
When The Team Actually Is Toxic

| Category | Value |
|---|---|
| Unsafe staffing | 80 |
| Toxic culture | 70 |
| Administrative chaos | 65 |
| Unreasonable workload | 60 |
| Location issues | 40 |
Sometimes it’s not your anxiety. Sometimes the place really is bad.
Red flags I’ve seen:
- Nurses openly say, “We don’t bother paging the doctor at night, nothing ever changes.”
- No backup when things hit the fan—just guilt and blame.
- Administration more worried about numbers than patient safety, and proud of it.
- You’re expected to quietly cover unsafe numbers of patients because “you’re locums and getting paid well.”
You are not obligated to emotionally fix a broken system as a temporary doctor. Your job is to be safe, professional, and not destroy yourself to compensate for structural dysfunction.
You’re allowed to:
- Call your agency or recruiter and say, “This is unsafe; I need support or I’m out.”
- Shorten an assignment if things are truly bad.
- Document concerns calmly and clearly (email to leadership, risk management).
Being locums gives you one insanely underrated power: the ability to leave. Staff often can’t. You can. Don’t forget that.
Quiet Mindset Shifts That Make This Easier

You’re not going to anxiety-manage your way into feeling 100% comfortable as a locum everywhere. That’s not real. But there are a few mental shifts that help a lot.
You’re not auditioning for your worth as a doctor every assignment.
You’re doing a specific job, in a specific environment, for a limited time. That’s it. Bad fit ≠ bad doctor.It’s okay if some people never like you.
You don’t need unanimous approval. You need enough trust that care is safe and you’re not miserable. That’s the bar.You’re allowed to protect your energy.
Being kind and professional doesn’t mean being endlessly accommodating. “No, I can’t pick up that extra shift. I’m already at my safe limit,” is valid.Being the outsider has upsides.
You’re less tangled in politics. Less dragged into old grudges. Sometimes staff tell locums the truth they won’t tell their own leadership because you’re… disposable. Use that information to practice medicine more clearly.
The Bottom Line
You’re not broken for feeling like the outsider doctor. Locums, especially right out of residency, amplifies every insecurity you already had and throws you into new systems that confirm your worst fears—for about a week.
Then the pattern usually becomes clear:
- You show you’re safe and respectful.
- You find 2–3 allies who don’t hate you.
- You adjust a few small workflow things.
- You stop feeling like you’re on trial 24/7.
You will not nail every assignment. Some teams will stay cold. Some places will be bad enough that leaving is the right move.
But your value as a physician is not defined by the most skeptical nurse on your first day, or the most chaotic hospital that hired a locum out of desperation.
Two or three things to remember when you’re spiraling before day one:
- You don’t have to be perfect. You have to be safe, reachable, and not a jerk.
- You’re allowed to say “I’m new here, walk me through how you do this.” That doesn’t make you weak; it makes you competent.
- Being locums means you can walk away from truly toxic environments. That’s power, not failure.


















